Iron supplements rank among the most commonly prescribed treatments for iron-deficiency anemia, a condition affecting millions worldwide. Yet despite their effectiveness at rebuilding depleted iron stores, these supplements come with a notorious reputation for causing gastrointestinal distress—particularly nausea that can make taking them feel like a daily battle. If you’ve ever started an iron supplement regimen only to find yourself dreading each dose due to persistent queasiness, you’re certainly not alone. Understanding why iron supplements trigger this unpleasant response involves exploring the complex chemistry happening inside your digestive system and the cascading effects those chemical processes have on your stomach lining.
The connection between iron supplementation and nausea isn’t simply a matter of personal sensitivity—it stems from specific physiological mechanisms that occur whenever iron enters the gastrointestinal tract. From the moment an iron tablet dissolves in your stomach, a series of chemical reactions begins that can irritate sensitive tissues, trigger inflammatory responses, and activate the body’s nausea pathways. The good news is that understanding these mechanisms empowers you to take practical steps toward reducing discomfort while still receiving the therapeutic benefits your body needs. This guide explores the science behind iron-induced nausea, examines the factors that influence its severity, and provides actionable strategies for managing this common side effect.
The Chemical Reaction Triggering Iron Supplement Nausea
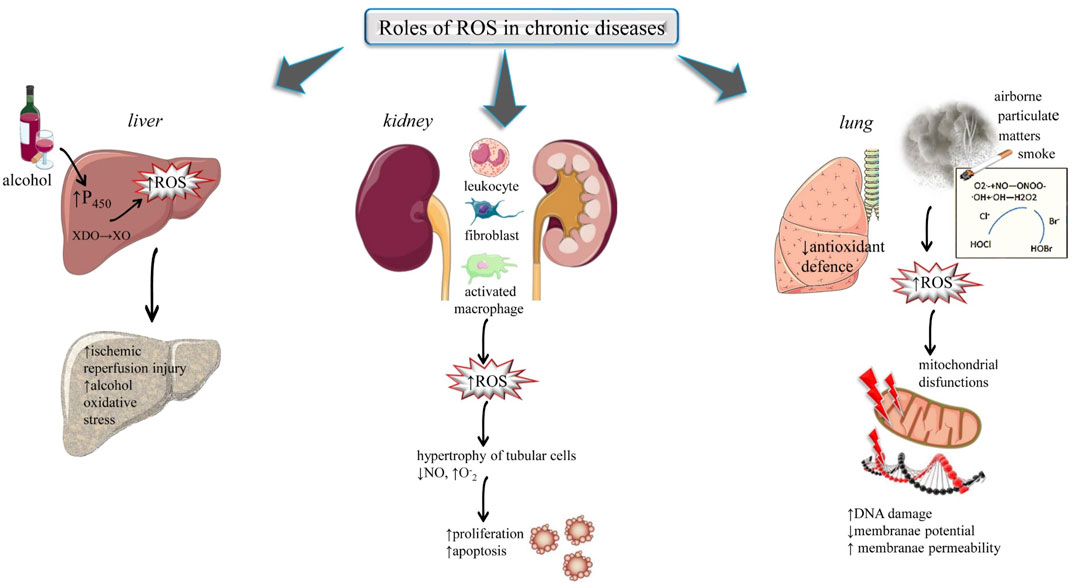
How Iron Oxidation Creates Free Radicals
The primary driver of nausea from iron supplements lies in iron’s tendency to undergo oxidation. When you ingest iron in its ferrous form (Fe²⁺), your body immediately begins converting it to the ferric form (Fe³⁺). This oxidation process doesn’t happen quietly—it generates reactive oxygen species, including highly unstable molecules called free radicals that attack delicate tissues throughout your upper digestive system.
These free radicals specifically target the lipids comprising cell membranes in your gastric epithelium—the protective lining of your stomach. When free radicals attack these cell membranes, they trigger inflammatory responses that compromise your stomach’s natural protective barriers. The result is exposed nerve endings and irritated mucosal tissue that collectively signal to your brain that something harmful has been ingested. This signaling pathway leads directly to the sensation of nausea, as your body’s defense mechanisms attempt to protect you from what it perceives as a toxic substance.
Physical Damage from Iron Particle Deposition
Beyond generating free radicals, the iron oxidation process leads to actual physical deposition of crystalline iron particles within your gastric and duodenal mucosa. Research examining tissue samples from patients experiencing iron-related gastrointestinal symptoms has consistently found these crystalline deposits concentrated in areas showing the most significant tissue damage. The pattern is remarkably consistent: wherever iron particles come into sustained contact with your stomach lining, corresponding areas of erosive damage appear.
This direct physical and chemical injury explains why nausea from iron supplements often accompanies other symptoms like epigastric pain, heartburn, and stomach cramps—the entire upper gastrointestinal tract is experiencing genuine tissue-level irritation. Unlike a simple upset stomach, this condition involves actual microscopic damage to your digestive lining that triggers your body’s protective nausea response.
Recognizing Iron Pill Gastritis: More Than Just Nausea

Identifying Tablet-Specific Stomach Damage
Iron pill gastritis represents a specific clinical condition resulting from oral iron supplementation in tablet form. Unlike general stomach upset, this condition involves actual inflammation of the gastric mucosa directly attributable to how iron tablets behave once they enter your digestive system. When a solid iron tablet encounters gastric acid, it begins dissolving and releasing concentrated iron ions that oxidize and precipitate out of solution. Unlike liquid formulations that distribute evenly throughout stomach contents, tablets create focal points of extremely high iron concentration where they make contact with your stomach lining.
Endoscopic examinations of patients with iron pill gastritis typically reveal multiple gastric erosions and sometimes small ulcers in the gastric antrum—the lower portion of the stomach where tablets tend to settle. Biopsy results consistently show iron-rich material adherent to the epithelial surface, with special staining techniques confirming excessive iron deposition in precisely those areas displaying the most tissue damage. If you experience persistent nausea accompanied by dark-colored stools or worsening anemia despite iron therapy, you should consult your healthcare provider about the possibility of iron pill gastritis.
Why Liquid Iron Causes Less Nausea Than Tablets
The difference between tablet and liquid iron formulations regarding nausea is striking and well-documented. Liquid iron supplements produce significantly less epithelial injury because they cannot concentrate within the gastric mucosa the way tablets do. Studies comparing outcomes have shown that even high serum levels of liquid iron do not produce the mucosal erosion observed with equivalent doses of iron in tablet form. This dramatic difference occurs because liquid iron disperses uniformly throughout stomach contents, providing more gradual exposure rather than the intense localized irritation that tablets create.
For patients who experience persistent nausea despite trying other strategies, switching from tablet or capsule iron to a liquid formulation may provide meaningful relief. While liquid iron supplements may require larger volumes to deliver equivalent elemental iron, the reduced localized irritation often makes this trade-off worthwhile for patients struggling with tablet-related nausea.
How to Reduce Iron Supplement Nausea Immediately
Optimizing Your Dosing Schedule
Taking iron with food represents the most effective immediate strategy for reducing nausea. While iron absorbs optimally on an empty stomach (about one hour before eating or two hours after meals), this timing also maximizes gastrointestinal irritation. Taking iron with a small meal substantially reduces nausea for most people, though it modestly decreases absorption—a practical trade-off that improves treatment adherence.
Try these timing adjustments:
– Take iron with simple, easily digestible foods like crackers or toast
– Avoid rich, spicy, or fatty foods when taking iron supplements
– Space iron doses at least two hours away from dairy products, antacids, or calcium supplements
– Consider taking iron with vitamin C (like orange juice) to boost absorption
– Drink eight ounces of water with each dose to help distribute iron throughout your stomach
Effective Nausea Relief Strategies
When nausea strikes after taking iron, several immediate relief approaches can help you manage symptoms:
For acute nausea:
– Lie down with your head elevated for 30-60 minutes after taking iron
– Try ginger tea or ginger candies, which have natural anti-nausea properties
– Practice slow, deep breathing to calm your nervous system
– Apply a cool compress to your forehead or neck
– Wait 15-20 minutes before attempting to eat if nausea occurs
If nausea progresses to vomiting, maintaining hydration becomes critically important. Take small, frequent sips of water or electrolyte solutions. Watch for signs of dehydration including reduced urine output and dark, strong-smelling urine. Patients taking oral contraceptives should be aware that vomiting may compromise contraceptive effectiveness and should consult their healthcare provider about appropriate precautions.
Long-Term Solutions for Iron Supplement Tolerance
Finding Your Ideal Iron Formulation

The specific chemical form of iron in your supplement significantly influences how likely it is to cause nausea. Ferrous sulfate, the most commonly prescribed formulation, tends to produce more gastrointestinal side effects than alternatives like ferrous gluconate or ferrous fumarate. Ferrous gluconate contains less elemental iron per tablet (approximately 12% compared to 20% in ferrous sulfate), meaning patients may need to take more tablets to achieve equivalent iron absorption but often experience reduced gastrointestinal symptoms.
If you consistently experience nausea with one type of iron supplement, discussing alternative formulations with your healthcare provider may provide a simple solution. Some patients find that simply switching to a different iron formulation resolves persistent nausea without requiring any other changes to their regimen.
Building Gradual Tolerance to Iron Supplements
Many patients develop tolerance to iron supplementation over time, with gastrointestinal symptoms often diminishing significantly after the first few weeks of consistent use. This adaptation may reflect gradual toughening of the gastric mucosa or adjustment of the body’s nausea pathways. To build tolerance:
- Start with a lower dose and gradually increase to your prescribed amount
- Take iron every other day initially, then progress to daily dosing
- Keep a symptom diary to identify patterns and triggers
- Pair iron supplementation with probiotic-rich foods to support gut health
- Consider taking iron at bedtime if nausea interferes with daily activities
When to Consider Alternative Iron Treatments
Evaluating Intravenous Iron Therapy
For patients who cannot tolerate oral iron despite trying various formulations, timing strategies, and dietary modifications, intravenous iron therapy offers an effective alternative that bypasses the gastrointestinal tract entirely. This approach eliminates nausea and other digestive side effects while delivering iron directly into the bloodstream where it can be immediately utilized.
Intravenous iron is typically reserved for patients who:
– Cannot absorb oral iron adequately due to gastrointestinal conditions
– Cannot tolerate any oral formulation despite concerted management efforts
– Require rapid iron repletion that oral supplements cannot provide quickly enough
– Experience persistent iron pill gastritis or other complications
While intravenous iron is more expensive than oral supplements and requires visits to healthcare facilities for administration, it provides life-changing relief for patients whose iron deficiency anemia remains untreated due to intolerable side effects from oral supplements.
Maintaining Treatment Adherence for Complete Recovery
Blood counts typically return to normal after approximately two months of consistent iron therapy, though treatment should continue for an additional six to twelve months to fully replenish depleted bone marrow stores. Premature discontinuation of iron therapy due to intolerable nausea represents one of the most common causes of treatment failure and subsequent relapse of iron deficiency anemia.
Working proactively with your healthcare provider to anticipate and manage side effects improves the likelihood of successful treatment completion. Don’t hesitate to report persistent nausea or other side effects—your provider can help you develop personalized strategies based on your individual circumstances, lifestyle factors, and the severity of your iron deficiency.
Understanding why iron supplements cause nausea transforms this frustrating side effect from an inexplicable problem into a manageable challenge with clear solutions. By recognizing the chemical processes driving your symptoms and implementing targeted strategies to mitigate them, you can successfully navigate iron supplementation while minimizing discomfort. Whether through formulation changes, timing adjustments, or in some cases alternative delivery methods, relief from iron-induced nausea is achievable. The key lies in approaching your treatment proactively, communicating openly with your healthcare provider, and remaining committed to the goal of restoring your body’s iron stores to healthy levels.