Women in their 40s and beyond increasingly search for solutions to manage hormonal changes as they approach perimenopause and menopause. DHEA supplements have emerged as a popular option, with manufacturers claiming benefits for everything from youthful skin to improved mood and vitality. This naturally occurring hormone, produced primarily by your adrenal glands, serves as a building block for estrogen and testosterone production in your body. As you age, your DHEA levels decline steadily—by about 2% annually after your twenties—creating the theoretical foundation for supplementation. But what does scientific evidence actually reveal about the benefits of DHEA supplements for women? Understanding the gap between marketing claims and research findings is crucial before adding this hormone precursor to your wellness routine.
The supplement market offers DHEA in various forms including tablets, capsules, topical creams, and transdermal gels, each promising different absorption rates and effects. Yet the reality is that DHEA research shows mixed results, with some potential benefits countered by significant safety concerns. This article examines what current studies actually prove about DHEA supplementation for women, separating evidence-based findings from hype while highlighting serious risks that demand your attention before considering this supplement.
Why Your DHEA Levels Naturally Decline After Age 30
Your body produces DHEA most abundantly during your twenties and thirties, with levels peaking around age 25. After this point, production decreases steadily by approximately 2% each year, resulting in significantly lower levels by the time you reach menopause. This natural hormonal shift forms the scientific rationale behind DHEA supplementation—replacing what your body no longer produces in youthful amounts. However, DHEA functions as a precursor hormone, meaning your body converts it into other essential hormones including estrogen and testosterone through complex enzymatic processes.
Individual variation in hormone conversion explains why women experience dramatically different effects from the same DHEA dose. Some women notice significant hormonal changes while others see minimal effects, making standardized dosing recommendations challenging. Your unique genetic makeup, current health status, and existing hormone levels all influence how your body processes supplemental DHEA. This variability matters immensely when weighing potential benefits against possible side effects, as your personal response could range from beneficial to problematic.
Visible Skin Improvements Documented in Clinical Studies

Research specifically examining DHEA’s effects on aging skin shows some of the most consistent findings for women considering supplementation. A clinical study with elderly participants revealed measurable improvements in skin hydration and firmness after several months of DHEA use. Participants also experienced a noticeable reduction in age spots, suggesting tangible cosmetic benefits. These skin-related improvements make sense biologically, as your skin contains DHEA receptors and responds directly to hormonal changes throughout your life.
As estrogen and DHEA levels decline during menopause, your skin typically loses elasticity, becomes thinner, and heals more slowly from damage. Topical DHEA applications have demonstrated particular promise in clinical settings for addressing these specific menopausal skin changes. While oral supplementation effects vary considerably based on individual metabolism, the dermatological benefits represent one of the more evidence-supported applications of DHEA for women. However, expecting comprehensive anti-aging effects throughout your entire body would significantly overstate what current research actually supports.
Mood Stabilization During Perimenopause Transition
One of the more promising research areas for DHEA supplementation involves emotional well-being during hormonal transitions. Studies indicate slight but measurable benefits for women experiencing mood swings and depressive symptoms during perimenopause and menopause. The hormonal turbulence of this life stage affects neurotransmitter function, potentially contributing to anxiety and emotional instability as estrogen levels fluctuate. DHEA’s role as a hormone precursor suggests it may help modulate these fluctuations through its conversion pathways.
Women reporting mood improvements typically notice better emotional regulation and reduced frequency of low mood episodes after consistent supplementation. However, research doesn’t support DHEA as a primary treatment for clinical depression or anxiety disorders. If you have bipolar disorder or a history of manic episodes, DHEA supplementation could potentially worsen your condition and increase manic episode risk. Always consult your healthcare provider before using DHEA for mood support, especially if you’re taking psychiatric medications or have pre-existing mental health conditions.
Vaginal Tissue Restoration for Menopausal Women

Among the most substantiated benefits of DHEA supplements for women involves relief from vaginal atrophy symptoms. This common menopausal condition causes thinning, drying, and inflammation of vaginal tissues due to declining estrogen levels. The resulting discomfort, pain during intercourse, and increased infection risk significantly impact quality of life for many postmenopausal women. Clinical research demonstrates that DHEA supplementation can improve vaginal epithelium thickness and moisture levels through local conversion to estrogen within vaginal tissues.
Women using DHEA for this purpose typically apply it topically as a vaginal insert rather than taking oral supplements. Studies show measurable improvements in tissue health and symptom relief within weeks of consistent use. While the evidence remains less extensive than for FDA-approved topical estrogen treatments, DHEA represents a promising alternative for women seeking non-estrogen options or those who cannot use conventional hormone therapy. If you’re experiencing vaginal atrophy symptoms, discuss DHEA alongside other evidence-based treatments with your healthcare provider to determine the safest, most effective approach for your specific situation.
Muscle Strength Claims Lack Scientific Backing
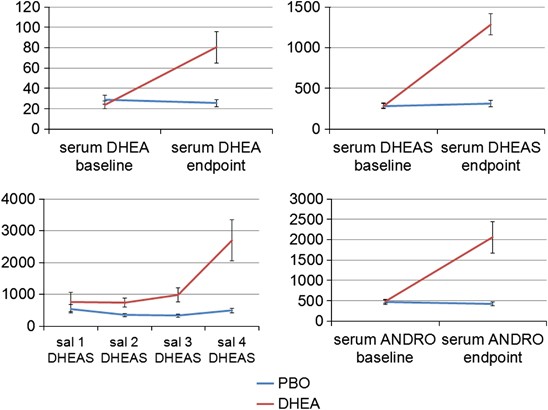
Despite aggressive marketing positioning DHEA as a performance enhancer, research consistently fails to support these claims for women. Multiple controlled studies across different age groups demonstrate that DHEA supplementation does not produce statistically significant improvements in muscle strength or physical performance. This finding directly contradicts supplement manufacturers’ promises of enhanced athletic ability or easier muscle building.
The National Collegiate Athletic Association’s ban on DHEA for competitive athletes reflects ongoing concerns about potential performance effects, yet scientific evidence doesn’t substantiate meaningful benefits. If you’re taking DHEA hoping to improve fitness results, you’re likely wasting money that would be better invested in proven strategies like consistent strength training, adequate protein intake, and proper recovery. The financial cost of DHEA supplements combined with their unproven performance benefits makes them a poor investment for most women pursuing physical fitness goals.
Inconsistent Product Quality Across Supplement Brands

When considering DHEA supplements, you must account for significant quality control issues throughout the supplement industry. Independent testing reveals alarming inconsistencies in actual hormone content compared to labeled amounts on DHEA products. Some supplements contain substantially less DHEA than advertised, rendering them potentially ineffective, while others contain more than labeled, creating risk of excessive hormone exposure.
Always choose DHEA products certified by independent testing organizations like ConsumerLab, NSF International, or USP Verified. These third-party verifications ensure dosage accuracy and absence of harmful contaminants. Even with certified products, remember that supplement manufacturers aren’t required to prove efficacy or safety before marketing their products in the United States. This regulatory gap places the burden of research and product selection squarely on your shoulders as a consumer.
Hormone-Sensitive Cancer Risks Demand Serious Consideration
DHEA functions as a prohormone with androgenic properties, meaning supplementation can increase androgen levels and produce steroid-like effects on your body tissues. Most significantly for women, research indicates that DHEA supplementation may increase the risk of developing hormone-sensitive malignancies including breast cancer and ovarian cancer. If you have existing cancer, a history of cancer, or elevated risk factors, you should absolutely avoid DHEA supplementation.
Women with high cholesterol or cardiovascular concerns face additional risks, as DHEA may reduce high-density lipoprotein (HDL) cholesterol—the “good” cholesterol that protects against heart disease. Common side effects include oily skin, acne development, and unwanted male-pattern hair growth (hirsutism) resulting from DHEA’s conversion to testosterone. These cosmetic effects can be distressing and may outweigh any potential benefits for many women.
Who Must Avoid DHEA Supplements Entirely
Certain women should categorically avoid DHEA supplementation due to elevated risk profiles. If you have hormone-sensitive cancers—past or present—DHEA could potentially stimulate cancer cell growth through its androgenic effects. Pregnant and breastfeeding women must also avoid DHEA completely, as hormonal effects could interfere with fetal development or infant health through breast milk transmission.
Women taking antipsychotic medications should be particularly cautious, as research shows DHEA may reduce the effectiveness of medications like clozapine. If you have bipolar disorder or a family history of mood disorders, DHEA supplementation could trigger manic episodes or worsen psychiatric symptoms. Before considering DHEA, disclose your complete medical history and current medications to your healthcare provider to determine if potential benefits outweigh your personal risk factors.
Mayo Clinic’s Official Recommendation Against Routine Use
The Mayo Clinic’s clinical assessment of DHEA supplementation recommends avoiding this supplement despite some preliminary research suggesting potential benefits. Their conservative stance emphasizes that while slight benefits have been observed for depression treatment and vaginal atrophy symptoms, the overall evidence supporting DHEA supplementation remains insufficient to justify the known and potential risks.
If you’re considering DHEA for menopause symptoms, mood concerns, or age-related changes, prioritize approaches with more robust safety and efficacy data first. Hormone replacement therapy under medical supervision, lifestyle modifications, and FDA-approved medications provide alternatives with more predictable outcomes. When discussing DHEA with your healthcare provider, focus on your specific symptoms, risk factors, and realistic expectations rather than marketing claims.
Women who decide to try DHEA despite the risks should implement strict safety protocols: verify third-party testing, start with the lowest possible dose, monitor for side effects, and schedule regular follow-up appointments with their healthcare provider. Maintaining realistic expectations while prioritizing evidence-based treatments ensures you make the safest possible choices for your long-term health and well-being.