If you’ve started taking fiber supplements only to find your constipation getting worse instead of better, you’re experiencing a frustrating paradox that affects millions. Contrary to popular belief, fiber supplements like psyllium husk and methylcellulose can actually trigger or worsen constipation for certain individuals. Research shows that patients already taking fiber supplements often present with the most severe constipation symptoms, creating a vicious cycle where the “solution” becomes the problem. This counterintuitive reality explains why you might feel more bloated, struggle with harder stools, and experience increased straining after adding fiber to your routine.
The conventional wisdom that “more fiber equals better digestion” fails for a significant portion of the population suffering from chronic idiopathic constipation. Clinical studies reveal that patients who reduce or eliminate dietary fiber experience dramatic improvements in bowel frequency and comfort, while those who continue high-fiber diets see no relief. If you’ve been diligently taking fiber supplements according to package instructions but still battle infrequent, difficult bowel movements, the supplements themselves might be the culprit rather than the cure.
This guide reveals the science behind why fiber supplements cause constipation in some people, how to identify if you’re affected, and practical steps to find relief by adjusting your approach. You’ll discover why reducing fiber—not increasing it—could be your path to regular, comfortable bowel movements.
The Fiber-Constipation Paradox
Healthcare providers consistently encounter patients with chronic constipation who are already following the standard advice to increase fiber intake through supplements and high-fiber foods. This pattern puzzled researchers enough to conduct a landmark study tracking 63 patients with idiopathic constipation over two years. The results shocked the medical community: patients who reduced or eliminated fiber saw dramatic improvements, while those who continued high-fiber diets showed zero progress.
The study divided participants into three groups: those who completely eliminated fiber, those who reduced but didn’t eliminate it, and those who continued high-fiber consumption. The outcomes were striking. Patients who stopped fiber entirely increased their bowel frequency from one motion every 3.75 days to one motion daily. Those who reduced fiber saw similar but less dramatic improvements. Most telling was the group that maintained high fiber intake—they remained stuck at approximately one bowel movement every 6.83 days with no improvement whatsoever.
This research proves what many patients have experienced firsthand: if you’re taking fiber supplements but still struggling with constipation, the supplements might be making your condition worse rather than better. Your body isn’t broken—you’ve likely been following advice that contradicts your specific digestive needs.
Why Fiber Supplements Worsen Constipation
Fiber supplements create constipation through three primary mechanisms that directly contradict common marketing claims. First, the bulking effect that’s supposed to promote regularity actually compounds evacuation difficulties when your colon is already struggling to move contents. Imagine adding more cars to a traffic jam—increasing stool bulk through fiber supplementation makes it harder, not easier, for your colon to process and eliminate waste.
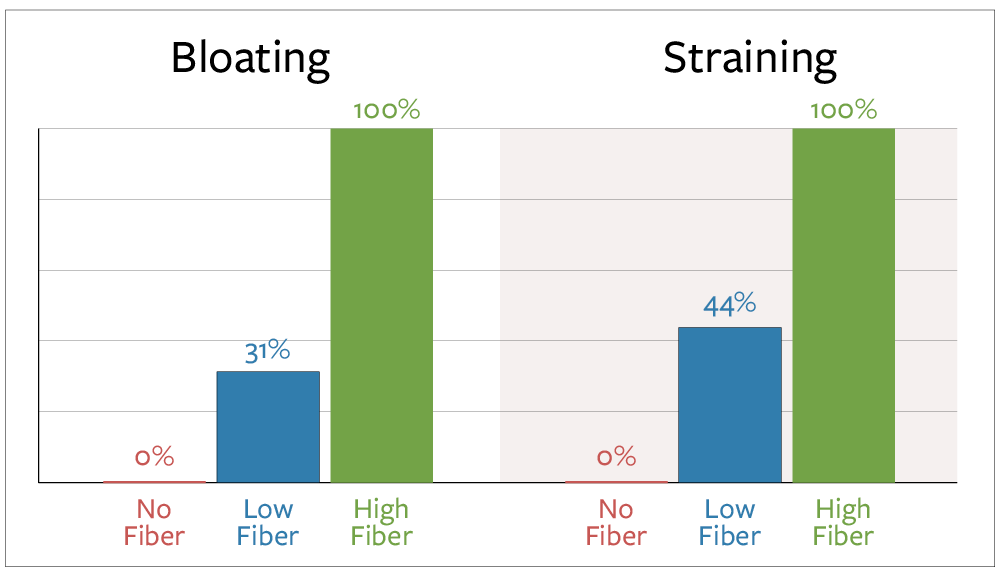
Second, fiber supplements significantly increase gas production through bacterial fermentation in your colon. As fiber reaches your large intestine, gut bacteria break it down, producing hydrogen, carbon dioxide, and methane. These gases get trapped by peristaltic movements, creating pressure against your intestinal walls. This explains why 100% of patients continuing high-fiber diets experienced bloating, compared to 31.3% on reduced-fiber diets and 0% with complete fiber elimination.
The Stool Moisture Myth
The most pervasive misconception about fiber supplements is that they soften stools by increasing moisture content. Research proves this wrong—stool moisture remains remarkably constant at 70-75% regardless of fiber or water intake. Your body maintains tight control over stool hydration, making the “fiber adds moisture” claim scientifically inaccurate.
When fiber supplements increase stool bulk without actually softening it, you end up with larger, harder-to-pass stools. For people whose constipation stems from evacuation difficulties rather than hard stools, fiber supplements create the perfect storm: bigger stools that require more straining to pass. This explains why many people experience anal bleeding and hemorrhoids despite faithfully taking fiber supplements—they’re literally forcing larger stools through a tight space.
Identifying Fiber-Related Constipation

You’re likely experiencing fiber-induced constipation if your symptoms worsened after starting supplements or if you’ve tried multiple fiber products without relief. Pay attention to these specific warning signs that indicate your supplements might be causing more harm than good:
- Constipation that persists or worsens despite regular fiber supplement use for more than two weeks
- Significant bloating and abdominal pain that intensifies after taking fiber supplements
- Blood on toilet paper related to straining during bowel movements
- Incomplete evacuation feelings even after significant straining
- A pattern where increasing your fiber dose makes symptoms worse rather than better
Signs You Should Reduce Fiber Immediately
Certain symptoms strongly indicate that fiber reduction—not supplementation—is your solution. If you experience anal bleeding during bowel movements, this signals mechanical trauma from passing overly large stools. Similarly, if you’ve tried at least two different fiber supplements without improvement, continuing to increase fiber is unlikely to help.
Patients who report worsening symptoms with each attempt to boost fiber intake should consider this a clear signal to change direction. The research shows patients who persisted with high-fiber diets despite medical consultation saw absolutely no improvement in symptoms—more of the same approach won’t yield different results.
Practical Steps to Reduce Fiber Intake
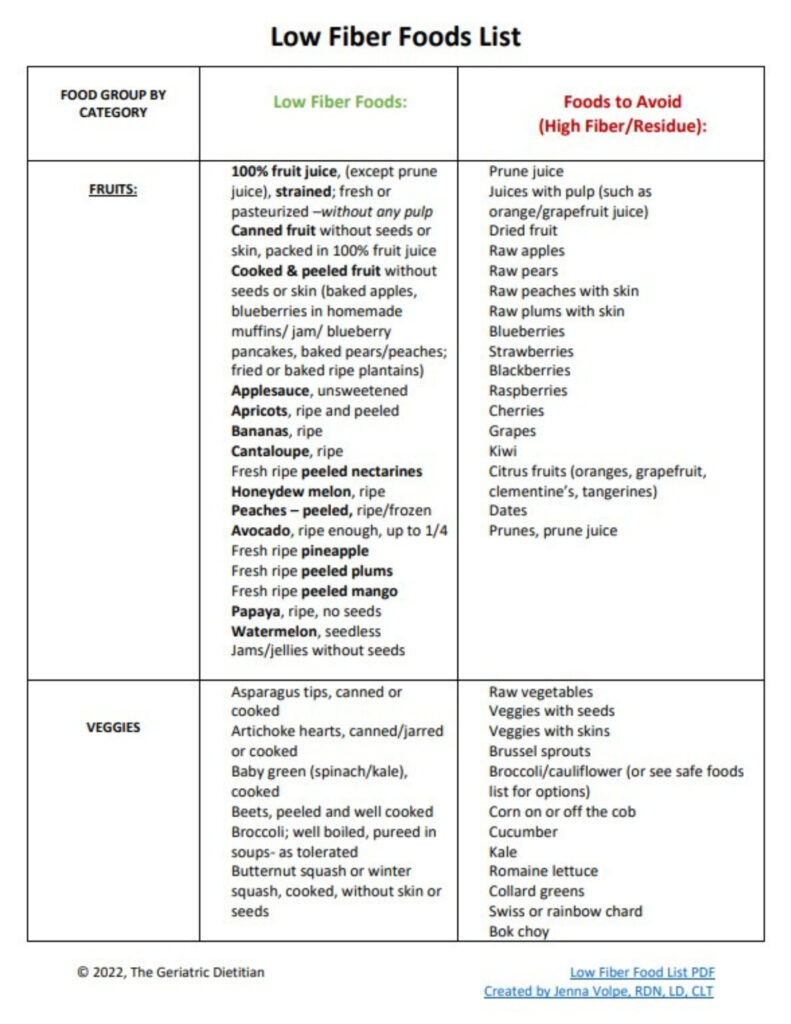
Start by eliminating all fiber supplements immediately and gradually reducing dietary fiber over 3-5 days to avoid sudden digestive disruption. During the initial two-week elimination phase, replace high-fiber foods with these low-fiber alternatives:
- Swap whole-grain bread for white bread and refined grain products
- Choose white rice instead of brown or wild rice varieties
- Remove skins from potatoes and other vegetables before cooking
- Select well-cooked, peeled fruits like bananas and melons instead of high-fiber options
- Replace beans and legumes with lean proteins like chicken, fish, eggs, and tofu
This transition period typically brings noticeable improvement within 3-7 days as your colon adjusts to processing smaller stool volumes. Most patients report reduced bloating first, followed by more regular bowel movements.
Critical Foods to Avoid During Fiber Reduction
To effectively address fiber-induced constipation, strictly avoid these high-fiber culprits during your elimination phase:
- All fiber supplements (psyllium, methylcellulose, wheat bran)
- Whole-grain breads, cereals, and pastas
- Raw vegetables with skins (carrots, cucumbers, tomatoes)
- Fruits with skins or seeds (apples, pears, berries)
- Nuts, seeds, and popcorn
- Legumes including beans, lentils, and soybeans
These foods contribute both soluble and insoluble fiber that can trigger the gas production and stool bulk that worsens your constipation. Even “healthy” high-fiber snacks can sabotage your progress during the critical elimination phase.
Managing the Transition Period
During the first few days of fiber reduction, you might experience temporary changes in bowel patterns as your digestive system adjusts. Some people notice slightly looser stools initially, while others experience a brief decrease in frequency. These transitional symptoms typically resolve within 3-5 days as your colon adapts to processing smaller volumes.
Stay well-hydrated with 8-10 glasses of water daily, but understand that hydration works differently without fiber. Water supports normal digestive function regardless of fiber intake, helping maintain optimal intestinal motility. Avoid carbonated beverages during this period as they can increase gas-related discomfort.
Long-Term Maintenance Strategies
After the initial two-week elimination phase, determine your personal fiber tolerance threshold. About 65% of study participants maintained complete fiber elimination long-term, while others found they could tolerate small amounts of specific fiber sources. Track your symptoms carefully as you experiment with reintroducing minimal fiber:
- Start with 1-2 grams of fiber daily from a single source
- Wait 3 days before adding another fiber source
- Note any return of bloating, straining, or reduced frequency
- Return to complete elimination if symptoms recur
Your goal isn’t zero fiber forever—it’s finding the minimal amount that maintains comfortable, regular bowel movements without triggering symptoms. Many people settle on moderate fiber intake (10-15 grams daily) after the initial elimination phase, significantly less than standard recommendations but enough to prevent symptom recurrence.
When Fiber Reduction Isn’t Enough
While fiber reduction solves constipation for many people, some require additional strategies. If you’ve eliminated fiber for four weeks without improvement, consult your doctor to rule out other causes like thyroid dysfunction, medication side effects, or structural abnormalities.
Combine fiber reduction with these complementary approaches:
– Establish regular meal times to trigger the gastrocolulic reflex
– Respond immediately to bowel movement urges rather than delaying
– Incorporate gentle physical activity like walking to stimulate motility
– Consider osmotic laxatives like lactulose if recommended by your doctor
Remember that fiber reduction works best for idiopathic constipation—constipation with no identifiable medical cause. If underlying conditions contribute to your symptoms, a comprehensive treatment plan addressing all factors will yield the best results.
Taking Control of Your Digestive Health
The path to relief from fiber-induced constipation starts with recognizing that conventional advice doesn’t apply to everyone. If you’ve been taking fiber supplements only to experience worsening symptoms, reducing rather than increasing fiber could be your solution. Track your current fiber intake and symptoms for one week to establish a baseline before making changes—this documentation will help you and your healthcare provider identify patterns and measure progress.
Your digestive system is unique, and what works for others might not work for you. By understanding why fiber supplements cause constipation for certain individuals and implementing a strategic reduction plan, you can break free from the cycle of worsening symptoms. The research is clear: for many people suffering from chronic constipation, less fiber—not more—is the key to regular, comfortable bowel movements.