If you’ve ever experienced uncomfortable bloating, gas, or digestive distress after meals and wondered why your body struggles with certain foods, enzyme supplements might hold the answer. Millions of people turn to these products seeking relief, but few understand precisely how do enzyme supplements work within the digestive system. The truth is that enzyme supplements contain concentrated versions of the proteins your body naturally produces to break down food into absorbable nutrients. Understanding the science behind how enzyme supplements work empowers you to determine whether they might benefit your digestive health and which types address your specific concerns.
This comprehensive guide reveals the precise mechanisms by which enzyme supplements support digestion, the different types available, conditions they treat, and practical considerations for effective use. Whether you’re considering pancreatic enzymes for a diagnosed condition, lactase supplements for dairy intolerance, or simply curious about digestive science, you’ll discover exactly how enzyme supplements work and how to use them effectively.
What Are Digestive Enzymes and Why Your Body Needs Them
Digestive enzymes are specialized proteins produced throughout your gastrointestinal system that catalyze the breakdown of food into smaller, absorbable molecules. Without adequate enzyme activity, your body cannot properly extract nutrients from even the most nutritious diet. The pancreas and small intestinal brush border represent the primary sites of enzyme production, though salivary glands and the stomach also contribute specific enzymes to the digestive process.
The human digestive system relies on three main categories of enzymes to process macronutrients. Proteolytic enzymes like trypsin and chymotrypsin break proteins down into smaller peptides and eventually individual amino acids that cells use for building and repairing tissue. Amylolytic enzymes, principally amylase, target carbohydrates and complex starches, converting them into simpler sugars like glucose that provide cellular energy. Lipolytic enzymes, led by lipase, handle the critical task of emulsifying and breaking down dietary fats into fatty acids and monoglycerides that your body can absorb.
When your body’s natural enzyme production becomes insufficient due to disease, genetic conditions, aging, or other factors, digestive enzyme supplementation provides essential support. How enzyme supplements work centers on replacing or supplementing these missing enzymes, allowing the digestive process to proceed normally and preventing malabsorption, nutritional deficiencies, and uncomfortable symptoms.
How Pancreatic Enzyme Supplements Aid Digestion
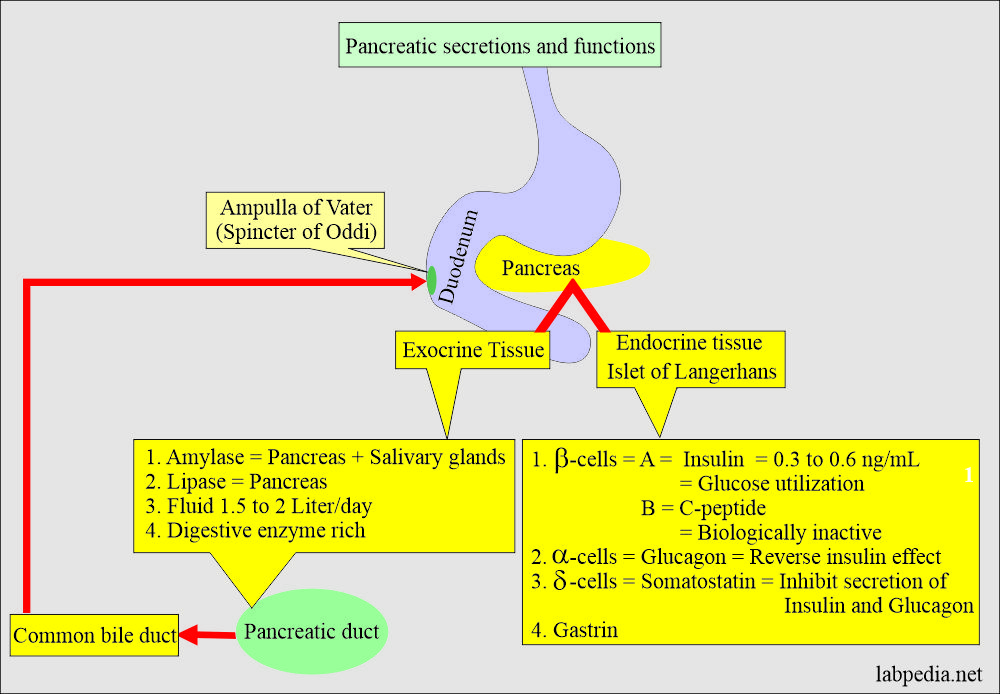
Understanding Exocrine Pancreatic Insufficiency
Exocrine pancreatic insufficiency (EPI) represents a serious condition associated with numerous pancreatic and extra-pancreatic diseases including chronic pancreatitis, cystic fibrosis, and pancreatic cancer. Patients experiencing unexplained weight loss, significant steatorrhea (fatty stools), or daily fecal fat excretion exceeding 15 grams on a standard diet are typically considered candidates for enzyme replacement therapy. These symptoms indicate that the digestive system is failing to extract adequate nutrition from food, necessitating intervention through pancreatic enzyme supplementation.
The Three-Pronged Mechanism of Pancreatic Enzymes

Pancreatic enzyme supplements work through three distinct but complementary mechanisms corresponding to the three major nutrient categories. Proteolytic enzymes in these supplements, primarily trypsinogen and chymotrypsinogen, break down dietary proteins into smaller peptide fragments and eventually into individual amino acids that pass through the intestinal wall. Amylolytic enzymes, represented by pancreatic amylase, target complex carbohydrates and starches, breaking them down into simpler sugars that the body can readily absorb. Lipolytic enzymes, principally lipase, handle the critical task of emulsifying and breaking down dietary triglycerides into free fatty acids and monoglycerides that the body can absorb and metabolize.
The exogenous pancreatic enzymes used in supplementation are primarily extracted from porcine or bovine sources, though lipase may also be synthesized from microbial sources. Animal studies have demonstrated that microbe-derived enzymes offer advantages including lower required dosage for effectiveness and a broader pH range of activity compared to animal-based counterparts, though porcine pancreatin remains the standard in many markets.
Protecting Enzymes for Effective Delivery
A critical aspect of how enzyme supplements work involves protecting the enzymes from degradation before they reach their site of action in the small intestine. The acidic environment of the stomach can significantly decrease the efficacy of exogenous enzyme supplementation, with lipase being particularly vulnerable as it becomes irreversibly denatured when exposed to pH levels of 4 or lower.
Enteric-coated preparations use specialized protective coatings that dissolve at higher pH levels, allowing the enzymes to pass through the stomach’s acidic environment intact and release only when they reach the more neutral environment of the duodenum. This technological advancement has significantly improved the effectiveness of pancreatic enzyme replacement therapy. Liprotamase represents a newer approach, containing purified and stable enzymes engineered to resist proteolysis and acid pH without requiring enteric coating, with clinical studies demonstrating effectiveness in patients with cystic fibrosis.
Lactase Supplements: Breaking Down Dairy Sugar
The Problem with Lactose Malabsorption
Lactase deficiency affects approximately 75 percent of individuals worldwide to some degree. This enzyme, produced by intestinal villi, specifically hydrolyzes lactose—the primary sugar found in milk and dairy products—into its component sugars galactose and glucose. High lactase concentrations are normally present in infants to digest breast milk or formula, but after weaning, lactase activity decreases in most people in a genetically-programmed fashion.
When individuals with lactase deficiency consume dairy products, undigested lactose reaches the colon where bacteria ferment it, producing gas and causing uncomfortable symptoms including bloating, gas, diarrhea, and abdominal discomfort. Lactose intolerance is defined specifically as the condition where this lactose malabsorption produces gastrointestinal symptoms.
How Lactase Supplements Prevent Digestive Distress
Lactase supplements work by providing the missing enzyme directly to the digestive system, either by adding the enzyme to milk before consumption or by taking capsules before eating dairy. When taken before consuming dairy products, the exogenous lactase begins breaking down lactose in the stomach and small intestine, preventing lactose from reaching the colon where it would otherwise be fermented.
The effectiveness of lactase supplements depends on several factors including the enzyme activity of the supplement, the timing of administration, the amount of lactose consumed, and individual variations in digestive physiology. Research shows that lactase supplements effectively decrease breath hydrogen—a marker of bacterial fermentation—when administered to lactose-intolerant individuals. However, with very high lactose loads (50 grams), even 6,000 international unit doses of beta-galactosidase may not improve digestion.
Comparing Lactase Sources and Potencies
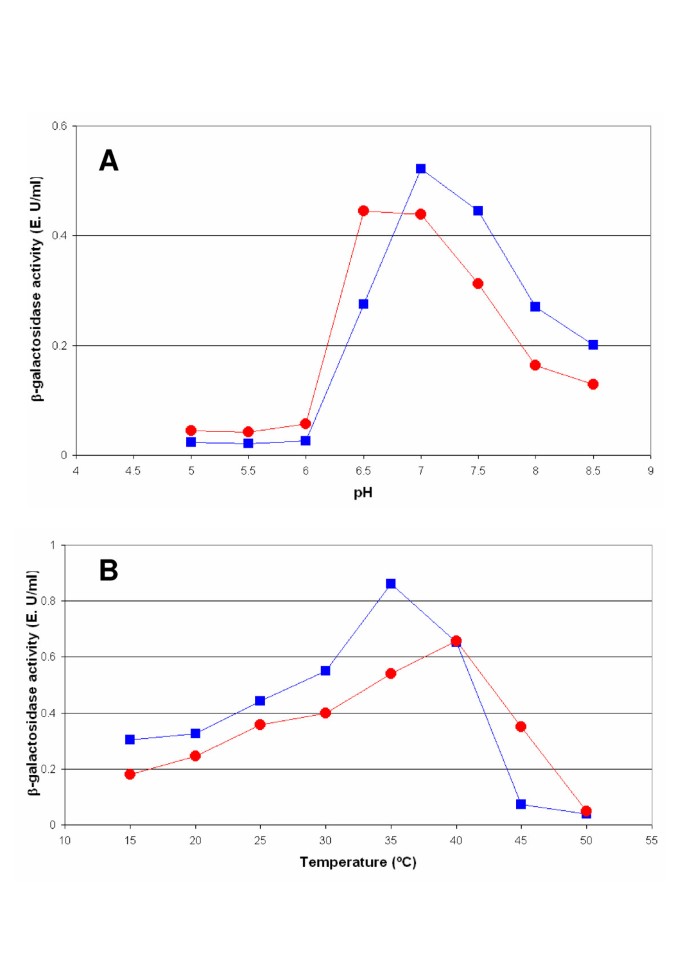
Enzymatic activity varies considerably among commercial lactase formulations. Some common lactase brands and their enzymatic activity include Silact with activity exceeding 30,000 units, Digerlat at 100,000 units, Lactaid at 9,000 units, and Dairy-Ease at 3,000 units. At equivalent doses, enzymes obtained from different microorganisms also display varying efficacy, with lactase derived from Kluyveromyces lactis demonstrating higher efficacy than lactase from Aspergillus niger.
These variations in enzyme activity explain why some lactase products may be more effective than others for individual users. Consumers selecting lactase supplements should pay attention to enzyme activity units rather than simply comparing capsule or tablet counts.
Choosing the Right Enzyme Supplement for Your Needs
Selecting the appropriate enzyme supplement requires matching the product type to your specific digestive needs. For exocrine pancreatic insufficiency, pancreatic enzyme replacement products containing trypsin, amylase, and lipase in appropriate ratios are essential. For lactose intolerance, lactase-focused products provide the specific enzyme that is deficient.
The measurement of enzyme activity varies depending on the specific enzyme and testing methodology. For amylase, measurements may be reported in USP units, Ph.Eur.U, or SKB units. Protease activity is typically measured in HUT or USP units, while lipase activity is measured in LU based on lipolytic activity utilizing olive oil as the substrate. Understanding these different measurement systems helps consumers make more informed comparisons between products.
Maximizing the Effectiveness of Enzyme Supplements
Timing and Administration Techniques
The effectiveness of enzyme supplementation depends heavily on proper administration timing and technique. Most pancreatic enzyme products should be taken during or immediately after meals to ensure proper mixing with food. Taking enzymes too early or too late in the meal reduces their contact with food substrates and diminishes effectiveness. For lactase supplements, taking the enzyme 15 to 30 minutes before consuming dairy-containing foods allows time for activation before lactose arrives.
The pH environment of the gastrointestinal tract plays a crucial role in enzyme function, and acidic conditions in the stomach can inactivate pancreatic lipase. Even enteric-coated enzymes require adequate bicarbonate secretion from the pancreas to maintain optimal pH in the duodenum.
Factors That Influence Enzyme Activity
Individual variation in the severity of enzyme deficiency, underlying disease characteristics, diet composition, and gastrointestinal anatomy all influence the optimal dosing strategy. Working with healthcare providers to determine appropriate dosing and monitor response is essential. The required daily dose varies considerably based on the etiology and severity of pancreatic insufficiency, as well as clinical features including age and body weight.
Storage conditions also affect potency, and products should generally be stored at room temperature away from excessive heat or moisture. Enzymes are proteins whose three-dimensional structure is essential for catalytic activity, and improper storage can lead to loss of function.
Safety Considerations and Potential Side Effects
Pancreatic enzyme supplements are generally well-tolerated when used at recommended doses, but potential side effects include gastrointestinal symptoms such as nausea, abdominal pain, and changes in bowel habits. Extremely high doses have been associated with fibrosing colonopathy, a rare but serious condition particularly observed in patients with cystic fibrosis. For this reason, doses should not exceed recommended maximums without close medical supervision.
Regular monitoring of patients on enzyme replacement therapy typically includes assessment of weight maintenance or gain, reduction in steatorrhea and other symptoms, and possibly laboratory measures of nutritional status.
The Future of Enzyme Supplementation Therapy
New frontiers of enzyme replacement are being evaluated for treating diseases beyond traditional enzyme deficiency states. Prolyl endopeptidases show promise for celiac disease because of their capacity to enhance the degradation of immunogenic gluten peptides in the gut. The combination of different enzymes and the addition of probiotics to enzyme supplements constitute intriguing therapeutic options that may improve outcomes for specific patient populations.
Research using fermented milk derivatives demonstrates increased lactose absorption and reduced symptoms of intolerance because yogurt microbes display intrinsic lactase activity. These findings support the potential benefit of probiotic additions to enzyme supplements, such as combining probiotics with lactase for lactose intolerance treatment.
Understanding how enzyme supplements work provides the foundation for appropriate use and realistic expectations. Whether you’re managing a diagnosed enzyme deficiency or exploring supplements for digestive comfort, the key lies in matching the right enzyme to your specific needs, administering it correctly, and maintaining realistic expectations about what supplementation can achieve. As research continues to advance our understanding of enzyme biology and delivery systems, the future holds promise for even more effective approaches to supporting digestive health through enzyme supplementation.